Lip filler correction begins with a thorough assessment of what has happened: whether filler has migrated beyond lip borders, accumulated unevenly, or lost the natural lip edge definition. Treatment depends on the specific problem identified. Dissolution, gradual reduction, or sometimes no intervention may be the right choice.
Why Lips Are Different
The lips occupy a unique position in facial anatomy. They are highly mobile, constantly moving with speech, eating, and expression. The skin is thinner and more delicate than the surrounding face, with a distinct demarcation between the lip vermillion (the coloured part) and the surrounding skin. The lip border itself is a precise anatomical boundary that defines lip shape and proportion. Blood flow to the lips is rich and rapid, which accelerates the movement of any injected material. The lips are also extremely expressive; any asymmetry, stiffness, or irregularity becomes immediately apparent during normal facial movement in a way that might not be obvious in other areas of the face.
Lip tissue has less structural support than cheeks or temples. There is no underlying bone; the lips sit over muscle and mucosa. This means filler has less containment and more opportunity to spread laterally if placed without precision. The lips also have significant lymphatic drainage, which affects how filler persists, breaks down, and redistributes over time. When filler correction is needed in the lips, these anatomical facts mean that standard correction approaches used elsewhere on the face often do not translate well.

How Lip Filler Problems Develop
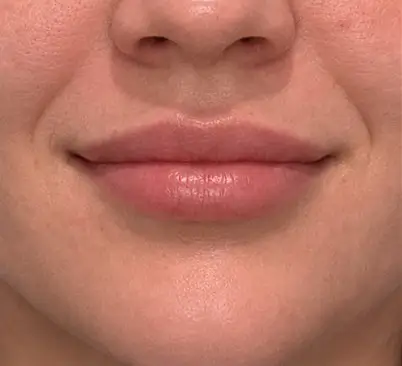
Lip filler complications typically develop through one or more of these pathways. The most common is filler migration beyond the lip border, where the material gradually spreads into the surrounding tissue, creating a blurred or swollen appearance above and below the natural lip line. This is not always immediately visible; it often develops over weeks to months as the filler integrates into the tissue and shifts with lip movement. Migration is more likely when the initial placement was too superficial, when too much volume was used for the lip size, or when filler was injected directly into muscle rather than into the dermal layer.
Overfilling is the second major pathway. Patients request fuller lips, and practitioners respond by injecting increasing volumes at each appointment. Over multiple treatments, this creates lips that do not look natural when at rest or during movement. The lips may appear swollen even when the patient is not speaking. The natural lip edge becomes blunted. Vertical lip lines may become more pronounced because the lip is overstretched. The lips may lose their natural colour definition because the filler compresses the thin epithelium.
Uneven distribution is also common. Filler may be concentrated in the centre of the lip with minimal augmentation at the corners, creating an imbalanced appearance. Or it may sit too superficially in patches, creating irregular texture. Asymmetry can develop if one side was injected with more volume or in a different plane than the other side. Some of these problems are visible immediately; others emerge over time as the filler settles and the lips adapt to the extra volume.
Assessment Before Any Correction
Before any correction is undertaken, a detailed assessment must establish what is actually present. This begins with observation of the lips at rest and during movement. How much volume is genuinely filler, and how much is swelling or the patient’s natural lip architecture? Where is the filler located, and how is it distributed? Is the lip border sharp or blurred? Are the lips symmetrical? Do they move normally, or does the patient experience restriction or stiffness? This assessment often requires a consultation period where swelling resolves, normal movement is observed, and the patient becomes comfortable describing their concerns without anxiety or frustration that might bias their perception.
Palpation of the lips is essential. The clinician gently feels the lip tissue to map where the filler is located, how dense it is, and whether it extends beyond what can be seen. Palpation helps distinguish between filler and natural tissue swelling. It can identify whether the filler is in the mid-dermis, in the superficial layer, or in the mucosa. This tactile assessment directly informs what correction strategy will work. Photography from multiple angles, including profile views and with the lips in movement, provides objective documentation and helps the patient see the specific issues rather than relying on their subjective impression.
Questioning is also critical. When was the filler injected? What was the treatment goal? How much was used at each visit? Has the appearance changed since injection? When does it look worst (morning versus evening, during social situations, with exercise)? Are there specific asymmetries that bother the patient most? Has the patient attempted any correction elsewhere? This history contextualises the current state and helps the clinician understand whether the problem is ongoing filler migration, settled filler in the wrong location, overfilling that needs gradual reduction, or a combination of these.
Understanding Filler Distribution and Border Integrity
During the assessment, the clinician maps out where the filler has settled. Has it stayed within the lip vermillion, or has it crossed the vermillion border into the skin above and below the lips? Does the filler respect the natural contours of the lip, or has it accumulated in a ridge or bulge? Is the density even across the lip, or are there nodules, dips, or irregular areas? The vermillion border integrity is particularly important because this is the line that defines where the lip begins and ends. When filler breaches this border on the upper lip, it creates a swollen appearance above the mouth. When it breaches below on the lower lip, it can obscure the natural transition from lip to chin and create a blurred or indefinite edge.
The assessment also considers whether the current filler distribution is aligned with the patient’s face. Do the lips suit the proportions of the rest of the face? Is the vertical dimension appropriate, or are the lips too tall and prominent? Does the volume complement the midface and jawline, or do the lips look isolated and disproportionate? Some filler problems are not truly “overdone” in absolute terms; they are overdone relative to that patient’s facial proportions and aesthetic goals. This distinction matters because it changes the correction strategy. Dissolution might be appropriate if the filler is genuinely excessive, but gradual reduction and rebalancing might be more suitable if the problem is one of proportion rather than volume alone.
Assessing Movement and Function
How the lips move during normal facial expression is a crucial part of assessment. Ask the patient to smile, purse the lips, speak, and perform exaggerated lip movements. Watch whether the movement is full and natural or whether the lips seem stiff or restricted. If the filler has been injected into muscle rather than dermal tissue, it may interfere with the normal contraction of the orbicularis oris muscle, the circular muscle that controls lip movement. This can create lips that do not move symmetrically, or that lack expression and seem artificial.
The patient’s subjective experience of movement is also important. Do they experience numbness, tingling, or altered sensation? Can they eat, drink, and speak without discomfort? Some patients with lip filler report that their speech is affected, or that they are hyperaware of their lips during social interaction because the lips feel different than they did before treatment. These functional changes may not be visible to an observer, but they significantly impact the patient’s quality of life and inform whether the filler should be removed even if the aesthetic appearance is not severely compromised. In some cases, patients with apparent aesthetic success report that they would prefer to have the filler dissolved because the functional impact outweighs the aesthetic benefit.
Tissue Quality and Skin Considerations
The texture and quality of the lip skin itself must be assessed independently of the filler. Has the filler caused the lip skin to become thin, crepey, or poorly hydrated? Are there fine lines more prominent now than before treatment? This is particularly important with hyaluronic acid fillers, because there is often an expectation that they improve hydration, but if the volume of filler is excessive, it can actually compress the epidermis and create a less healthy skin appearance. Some patients experience a change in lip colour or pigmentation; this can be due to the filler itself, to swelling and bruising that has persisted, or to changes in how light reflects off the altered lip contour.
Surface texture is also relevant. Are there palpable irregularities under the skin? Can the patient feel the filler with their tongue, or can you feel it on palpation? Some fillers, if poorly placed or if the body’s inflammatory response is pronounced, can create a grainy or nodular texture. This texture may or may not be visible to an observer, but it is uncomfortable for the patient. The assessment must distinguish between temporary swelling or roughness that will resolve on its own, and true texture issues that will persist and need intervention.
Symmetry and Proportion
Asymmetry is common in lip filler correction cases. The assessment must identify whether asymmetry existed before filler treatment, whether it was created or worsened by the filler, and whether it is significant enough to warrant correction. Some asymmetry is normal and natural; perfect bilateral symmetry in the lips is not a clinical goal and may actually look artificial. However, asymmetry that troubles the patient or that is noticeable during movement does warrant attention.
Proportion is assessed by comparing the lips to the rest of the face. The lip-to-chin ratio, the relationship between upper and lower lip height, and the position of the lips relative to the nose and face outline all matter. If the filler has created lips that are disproportionately full relative to the patient’s face shape, age, or stated goals, this is a correction issue even if the lip filler itself was technically well-placed. The assessment identifies whether the correction should focus on removing absolute volume, on rebalancing proportions, or on both. This distinction directly informs the treatment plan and outcome expectations.
Treatment Pathways: Dissolution
Dissolution using hyaluronidase enzyme is one correction option, but it is not the only one and it is not always the first choice. Hyaluronidase breaks down hyaluronic acid filler relatively quickly, over hours to days, allowing the lips to return towards their pre-filler state. This is valuable when the problem is significant migration, overfilling, or asymmetry that cannot be addressed through refinement alone. However, dissolution is not a precision instrument. It is difficult to dissolve exactly the right amount of filler; the enzyme works relatively indiscriminately once injected, and it is not possible to confine it perfectly to the areas where it is unwanted.
When dissolution is appropriate, it is usually performed in a staged approach rather than complete immediate dissolution. The first session dissolves a portion of the filler, and the lips are reassessed after two weeks to determine whether further dissolution is needed. This staged approach allows the patient’s natural lip architecture to become apparent gradually and allows the swelling from the dissolution process itself to resolve before deciding on the next step. Patients are counselled that their lips may look thinner than they anticipated once the filler is gone, and that this may change their perception of what was “overdone” and what was simply more volume than their natural baseline.
Treatment Pathways: Partial Reduction
Not all lip filler correction requires complete dissolution. In some cases, the lips simply have too much volume but the placement is acceptable and movement is good. In these situations, the patient can be monitored and allowed to continue their normal activities, letting the filler gradually integrate and settle. Many hyaluronic acid fillers are partially metabolised over months, and some patients find that allowing six to twelve months to pass results in a gradual improvement without intervention.
Alternatively, if the patient wants more active correction but does not want complete dissolution, the clinician can recommend waiting until the patient’s next treatment interval and then simply not replacing the filler. Some patients received repeated filler top-ups, and by stopping these top-ups and letting the existing filler gradually break down, the lips naturally return to a more appropriate volume without the need for dissolution. This approach requires patience and realistic expectations, but for some patients it is the most conservative and comfortable path to correction.
Treatment Pathways: Reset and Rebuild
In more complex correction cases, the best approach is a reset: dissolving the existing filler back to baseline or nearly baseline, waiting for the tissue to settle, and then, months later, carefully rebuilding with conservative volumes and more precise placement. This pathway is chosen when the problem is significant enough that partial correction is unlikely to satisfy the patient, but also when there is enough concern about tissue quality or filler location that proceeding directly with additional filler would compound the problem.
The reset approach has several advantages. It allows the lip anatomy to declare itself fully. Once the filler is gone, the clinician can see the patient’s true lip shape, volume, and borders without filler interference. Any tissue changes caused by the filler, such as thinning or loss of elasticity, can be evaluated. The patient can make a fully informed choice about whether they want to pursue re-treatment and under what parameters. The timeline between dissolution and rebuilding (typically two to three months) allows swelling to resolve completely and allows the patient to experience what their lips look like without filler, confirming whether they truly want additional treatment.
Post-Dissolution Lip Behaviour
After filler dissolution, the lips change in ways that sometimes surprise patients. First, swelling increases in the immediate aftermath of the dissolution treatment. The enzyme breaks down the filler, which causes a localized inflammatory response. The lips may be more swollen for two to seven days after dissolution than they were before. This acute swelling resolves gradually. Second, as the filler disappears, the lips often appear thinner than expected. This is because patients have become accustomed to seeing their lips with volume. The natural lip baseline, without any filler, may look small by comparison. Most patients report that their perception shifts over two to four weeks, and that lips that initially looked too thin become acceptable as they readapt to seeing their natural lips.
Texture can also change. Some patients report that the lip skin feels different after dissolution, sometimes smoother and sometimes slightly rougher. If the original filler had been partially integrated into the tissue or had caused inflammation, removal of the filler can leave the tissue temporarily irritated. For most patients this settles within weeks. Some patients report that they experience a heightened sensitivity to products applied to the lips, such as balms or lipsticks, during the first few weeks after dissolution. Fine lines that were previously plumped may become more visible. This is normal and often temporary as the lips hydrate and settle.
When Not to Refill Immediately
A critical principle in lip filler correction is that re-treatment should not happen immediately after dissolution or after identification of correction issues. Refilling immediately makes it impossible to see the patient’s true natural anatomy, and it risks perpetuating the same problems that required correction. The lips need time to fully settle, swelling needs to resolve, and the patient’s perception and satisfaction with their natural baseline need to stabilise. During this waiting period, the patient can also reflect on whether they truly want additional filler, or whether the experience of their lips without it has changed their preferences.
The waiting period also serves a clinical function. If the problem was migration, the clinician needs to understand whether the migration was due to placement technique, to the patient’s tissue characteristics, to the specific filler product used, or to the volume injected. These questions cannot be answered immediately; they require observation over time. If a patient returns for re-treatment weeks or months later, the new treatment can be performed with lessons learned from the previous experience. If the problem was overfilling, the waiting period gives the clinician and patient time to recalibrate expectations for what is “appropriate” volume. Many patients discover, after experiencing the correction or dissolution process, that they prefer a smaller volume than their pre-dissolution filler state suggests they wanted.
Building a Long-Term Lip Strategy
If re-treatment after correction is appropriate, it is framed as part of a long-term strategy rather than as a single augmentation. The strategy begins with clarity on goals: Does the patient want fuller lips than their natural state, or do they want to maintain their natural borders with subtle enhancement? Do they want enhanced definition, or enhanced volume, or both? Are there specific asymmetries they want to correct? What is the patient’s comfort level with being recognised by people who knew them before treatment, and how much change is acceptable?
Based on these goals, a conservative treatment plan is developed. Rather than targeting maximum volume, the plan targets a modest enhancement that respects the patient’s natural proportions and facial structure. The interval between treatments is extended: rather than annual top-ups, treatments are spaced at eighteen to twenty-four month intervals, with careful monitoring of how the filler settles and whether migration or complications develop. The volume at each treatment is lower than it would have been in the pre-correction scenario, based on lessons learned.
The strategy also includes clear communication about what the patient can expect as they age. Lips thin naturally with age; filler can maintain or enhance volume, but it cannot prevent the gradual changes that occur with time. A strategic approach means accepting that the lips will change over years and treating this as expected rather than as a failure of treatment. It also means being honest when a patient has reached a plateau of acceptable results and does not need further treatment, even if they could technically accept more volume.
Psychological Considerations and Managing Expectations
Lip filler correction often involves a significant shift in patient expectations and self-perception. Some patients feel relief when their filler is dissolved or reduced, and they report immediately feeling more like themselves. Others experience disappointment or grief; they had accepted the fuller lips as their new normal and are confronted with their natural baseline. Some patients feel regret about the years they spent with excessive or poorly placed filler. Others worry about what others will think of the change in their appearance. These psychological responses are real and valid, and they warrant acknowledgement and support during the correction process.
Setting realistic expectations before correction helps mitigate these challenges. The patient needs to understand that their natural lips, post-correction, may look different from both their pre-filler appearance and from their current filler appearance. The timeline for accepting this new (or returned) appearance can be weeks to months. They should know that refilling will be optional, not automatic, and that waiting months before deciding is a sign of wisdom rather than indecision. Patients are also counselled that correction does not erase the treatment history; once you have experienced fuller lips, it can be psychologically challenging to return to a smaller baseline. This is normal and something to anticipate and prepare for emotionally.
Outcome Expectations After Correction
The realistic outcome of lip filler correction is not restoration of a “before” state, but rather a balanced, functional, and sustainable result that addresses the specific problems identified during assessment. If the problem was migration beyond the lip border, the outcome is a lip with a clearer, more defined border and a reduction in the swollen appearance of the surrounding skin. If the problem was overfilling and loss of natural lip definition, the outcome is lips that can move freely and that look proportionate to the face. If the problem was asymmetry, the outcome is improved balance, though perfect symmetry is neither achievable nor desirable.
Patients should not expect their lips to look exactly as they did before filler treatment. Time has passed, the lips have changed, and the tissue has been affected by the filler experience. Some patients note that their lips have a slightly different texture, or that fine lines are more visible, or that the natural lip colour is slightly different. These are normal variations and typically resolve or become less noticeable over months. If re-treatment is chosen, the outcome is enhanced lips that are proportionate, symmetrical, stable, and aligned with the patient’s long-term aesthetic goals. The focus is on quality and sustainability rather than on maximum volume or dramatic change.
Frequently asked questions
Is lip filler correction painful?
Dissolution is similar in discomfort to injection; most patients experience mild stinging during the injection itself, which subsides quickly. No significant pain is expected. Swelling and mild tenderness in the hours after treatment are normal.
How long does it take to see the results of correction?
Changes are visible within hours to days, but the full effect takes two to three weeks as swelling resolves. If staged dissolution is performed, follow-up treatments may occur two weeks apart.
Can I dissolve just part of my lip filler?
Yes. Staged dissolution allows for partial removal of filler, so correction does not have to be all-or-nothing. Assessment and conservative approach determine how much is dissolved at each stage.
Will my lips look natural after filler is dissolved?
Your lips will return to their natural state prior to filler treatment. Whether this looks "natural" depends on your perception and your face’s proportions. Many patients find their natural lips look more in proportion once over-filled filler is removed.
How long should I wait before refilling my lips after correction?
A minimum of two to three months is recommended to allow swelling to fully resolve and to give you time to assess your true natural lips. Longer waiting periods allow for better decision-making and reduce the risk of repeating previous problems.
What if dissolution does not remove all the filler?
Staged approaches mean you can return for further dissolution if needed. Rarely, a small amount of filler may persist, particularly if it was placed very deep or if it has already partially integrated into the tissue. Assessment at each stage determines whether further intervention is needed.